Rethinking End of Life or Futile Care
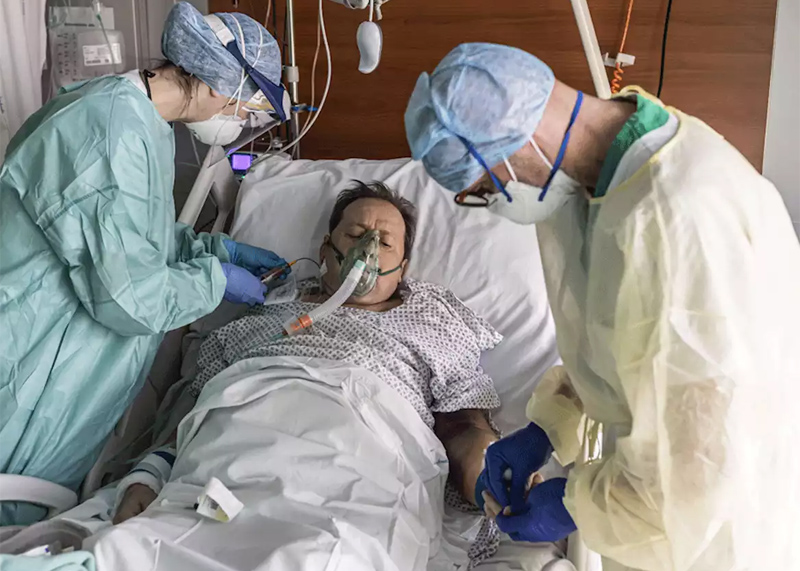
The Issue
As the death toll of the coronavirus pandemic mounts, physicians are encouraging Canadians to plan for serious illness and possible death now, rather than leaving family and medical staff to make those difficult decisions once they or their loved ones become near terminally ill. Many Canadian families are encountering the phenomenon of health-care rationing for the first time in their lives. For the moment, rationing is sporadic and confined to items like toilet paper and masks. However, how will we respond if rationing moves from consumables to life itself?
The COVID-19 pandemic has shed a light on many weaknesses of the world’s public-health systems. In Canada, where the national health-care system was stretched even before the expected COVID-19 surge, a conversation has begun about the need to direct health care resources to where they will be most effective and away from where they will not help. In some cases, this is opening the door to a long-delayed public conversation about the provision of “futile” care in a pandemic setting of limited resources.
What role do families, patients, and health-care providers as well as hospital administrators play in determining who gets futile care? Is there a need to update processes about end of life discussions? How close are we to allowing “death panels” and “do not resuscitate” (DNR) orders to be applied more aggressively in hospitals and nursing homes?
Ethics and Values Dilemmas

Given the finite number of beds in intensive care units, as well as respirators, masks, gowns and gloves, the harsh truth is that if there is a second wave, mass contagion on a broad scale, there will not be enough medical resources to sustain the lives of all who need care. There are certain situational end-of-life, health-care realities that should be acknowledged:
- In COVID-19 wave one, governments and their advisers worked to reduce the number of infections in the hope that they could prevent the overloading of our limited resources.
- An estimated 200,000 Canadian patients with symptoms other than coronavirus who were scheduled for treatment were denied services in the pre-occupation with “flattening the curve”—hundreds died as a result while empty hospital ICU beds designated for COVID-19 went unutilized.
- In wave two, medical staff and families in certain jurisdictions will most certainly need to exercise triage – put simply, the practice of prioritising access to scarce medical resources. Not everyone will be chosen for further treatment.
- Tracking, testing and tracing will need to effectively be allocated to reduce infection rates expected in the second wave of infection.
In Ethics Blog “Rationing Who Gets Care (April 1)” and “Cure versus Care: Flattening the Curve” (March 24), the harsh ethical realities behind abstract talk of medical treatment choices are explored. There is an upper limit in terms of equipment and trained personnel – there is just not an endless supply of either and no amount of money can solve that problem once the number of people seeking care exceeds the effective places available.
End of life care and infectious disease professionals suggest five necessary and helpful strategies:
1. Think and Communicate Proactively and Beyond Resuscitation

Good communication can facilitate the development of a comprehensive treatment plan that is medically sound and consistent with a seriously-ill patient’s wishes and values. A large majority of patients and close family members are open to discussing end-of-life issues with their physician. Most expect their physician to initiate such dialogue. More of such discussion time, however, should go beyond the narrow focus of resuscitation in order to address the many concerns shared by most dying patients and families: fears about dying, understanding prognosis, achieving important end-of-life goals, and attending to physical needs. Good open communications can allay fears, minimize pain and suffering, and resolve many end-of-life issues resolved comfortably, without conflict.
2. Not All Family Discussions Are Amiable
In the later stages of life of a health-compromised parent, many family members may often have very different conflicting opinions about what level of extraordinary care their dying parents would want. Sons and daughters acting as substitute decision-makers have very different genuinely-held expectations and care treatment goals they believe their frail parent would want followed. This is particularly troublesome when a treatment plan is incomplete, COVID-19 is the diagnosis, and the patient is incapacitated and unable to express his or her wants.
Having discussions around serious illness and death helps ensure people do not get unwanted or inappropriate care for a specific condition. For instance, even if you wanted CPR, you would not receive it if you were brain dead from a head trauma or stroke. This would be the case if that were the patient’s wishes and if they were known to the treatment team. Otherwise, the presumption of “full code” governs treatment decisions in Emergency and perhaps beyond.
One of the unspoken problems of critical care true since long before COVID is that the wrong care can be applied to the wrong person. For example, there are patients in ICU (intensive care units) on mechanical ventilation who never would have wanted that in the first place. Patients and families should do the necessary advanced planning for serious illness to ensure that they get the right care for them, and that their substitute decision makers have a less stressed experience filling that role.
3. Patents Wishes Can and Do Conflict with Those of Professional Health-Care Workers

Daily in most hospitals, ICU physicians and hospitals receive pressure to “save” people because the family insists. . The struggle with COVID-19 is a calculation few have encountered. in their lifetimes — how to weigh the “save at all costs” approach to resuscitating a dying patient when pitted against the real danger of exposing doctors and nurses to the coronavirus contagion. To the extent these conversations take place, they are being driven by the realization that the risk to staff amid dwindling stores of protective equipment — such as masks, gowns and gloves — may be too great to justify the conventional response when a patient “codes” and their heart or breathing stops.
Several large hospital systems in the United States — Atrium Health in the Carolinas, Geisinger in Pennsylvania and regional Kaiser Permanente networks —are looking at guidelines that would allow doctors to override the wishes of the coronavirus patient or family members on a case-by-case basis due to the risk to doctors and nurses, or a shortage of protective equipment, say ethicists and doctors involved in those conversations. At least to date, they apparently would stop short of imposing a do-not-resuscitate order on every coronavirus patient. The companies decline to comment.
4. New Frail Health COVID Decision-Making Realities
Some critical care consultants emphasize that, if health care teams risk their well-being in service of one patient, that can detract from the care of other future patients, which is unfair. One physician who asks not to be named, calls for a two physician solution– one directly taking care of a patient and one who is not, to sign-off on do-not-resuscitate orders. With this model, they both must document the reason for the decision, and the family must be informed but does not have to agree.
The Canadian Journal of Emergency Medicine, recently published a paper emphasizing that in certain scenarios amid the pandemic, patients may not want life-sustaining therapies, such as intubation, mechanical ventilation and hemodialysis– treatments that will not always be successful. Some hospitals in the U.S. are reportedly considering universal “do not resuscitate” orders for all patients with COVID-19. Dr. Merril Pauls, a professor in the department of emergency medicine at the University of Manitoba and chair of the bioethics committee at the Canadian Association of Emergency Physicians, is quoted as saying that he does not know of any hospitals in Canada that have enacted such policies.
5. Who Will Live Longer vs. A COVID Survival Choice?
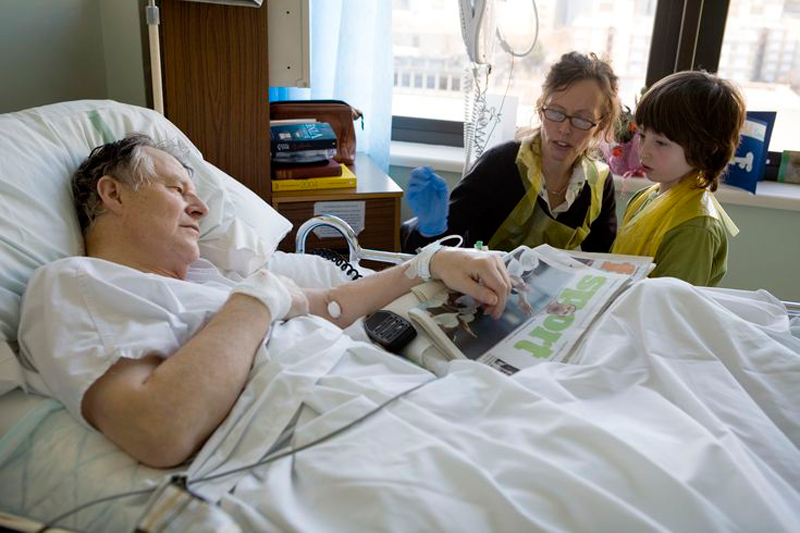
In a series of 15 focus groups among 324 people, Johns Hopkins researchers found that over half of health-care workers would use “live longer” as the first principle about who gets a ventilator in this pandemic, but barely a quarter of lay people would, preferring “survive current illness.” Few people liked a lottery, or “fewer life stages” or “first come, first served” or “value to others” as the first rationing principle.
Traditional advanced-care plans, which focus on end-of-life care for patients with terminal illnesses, are not very helpful in the current pandemic situation. People should now be planning for serious illness not only where there’s a possibility of death, but also survival. That’s because when people catch pneumonia from this new coronavirus, it is a serious but not necessarily fatal illness. Critical care providers will need to make decisions about whether to use life-sustaining measures when they do not know what the outcome for their patients will be.
Legal and Values Dimension

Faced with coronavirus, it is increasingly difficult to conclude that patients’ goals for care should be seen as routine, not scary or frightening. Roughly 30 per cent of the general population and 70 per cent of individuals who are very ill already have a plan like an advanced directive, a legal document outlining one’s care wishes. However, these plans, sometimes known as living wills, do not always reach front line health providers. Obstacles to effective communication include:
- (a) people not discussing plans with their lawyers, not all of whom take the time,
- (b) not discussing the plan with their doctors, and
- (c) stashing documents in places where others can’t access them. Some patients also do not inform hospital staff about their end-of-life wishes, possibly because they go the hospital intending to get well, not to die.
According to health professionals, there is a profound difference between preserving life on the one hand and merely extending the process of dying, on the other. The medical technology used in both cases is the same. Ethical discernment makes the difference. If pressure mounts on intensive care units, then we can expect more families and loved ones to be asked if continuing treatment is not only futile but also denying another person a chance of life. Who of us is prepared for such a conversation?
In recent years, Canadian jurisprudence and regulatory policies have given the impression of exalting patient and family desires over professional judgment and a just resource allocation. One case is McKitty v. Brampton Civic In some cases, these controversial developments have served to increase the provision of “futile”, costly, and potentially harmful care in intensive care units in Canada.
Medical regulators and governments have allowed the courts to lead on this issue and have mostly remained passive. With a pandemic upon us, however, the folly of neglecting a public debate on the appropriateness of this approach has become evident, as policy makers find their ability to manoeuvre around these challenging and emotionally charged issues constrained by a lack of public insight and input. Ontario has been the recent epicentre of much of this debate and the topic has generally provoked an acrimonious relationship between health-care providers and their medical regulator (the College of Physicians and Surgeons of Ontario (CPSO). The CPSO’s policy responses to cases such as Cuthbertson v Rasouli or Wawrzyniak v. Livingston have been questioned – some even casting doubt on their fundamental ethical soundness.
The COVID-19 crisis is now forcing a more urgent consideration of the issue. The provincial government in Ontario recently laid out criteria for allocation of resources (triage) on an objective basis. In some analysts minds, this raises the spectre of “death panels” that choose who lives and who dies.
According to analysts Lucas Vivas and Travis Carpenter, writing in Journal of Medical Ethics, these trying times have the potential to bring out all that is greatest in humanity. Medical regulators have a duty to support the front-line clinicians in their important work of educating and accompanying patients even while difficult decisions must be made. Now is the time for both governments and medical regulators to lead the broader public discussion on appropriate care and medical futility. Canada’s provincial governments, Ontario’s in particular, have displayed courage in defining limits and criteria for the provision of publicly-funded care – a resource that belongs to us all. It is time for the CPSO and other medical regulators to lead with the same alacrity.
None of this is meant to suggest that some lives are intrinsically more valuable than others. They are not –in theory, we patients are all equal in our possession of fundamental dignity. Nor does any resort to mandated triage imply indifference to the wellbeing of those who cannot receive life-saving care. Those who miss out will be given the most compassionate care available as they die. This is not the same as saying that nobody need suffer.
Promoting the idea that we should be doing end-of-life care plans is not going to be helpful to critical care doctors when they don’t know if this may involve a patient’s death wish. We should spare a thought for those who may be called to make these difficult treatment decisions. The physical, emotional and spiritual toll will be immense.
Conclusion

COVID-19 has accentuated the life and death stresses on families and health-care professionals. There needs to be a broad public discussion about appropriate care and medical futility. No amount of reason or decision-making aids or counselling for essential-care, health-care providers can prevent the abrasive effects on the human psyche of triage or saying good-bye to a family member. Medical professionals, families, health-care regulators, and members of the wider community will all need maximum compassion and support as well as our support. There, but for faith or chance, go you and I.
Further Reading:
Washington Post – Hospitals consider universal do-not-resuscitate orders for coronavirus patients:
https://www.washingtonpost.com/health/2020/03/25/coronavirus-patients-do-not-resucitate/
EthicScan Blog – Why are we failing health-care workers?
http://ethicscan.ca/blog/2020/04/22/why-are-we-failing-health-care-workers/:
Scientific American – What if Two COVID-19 Victims Need Ventilators and Just One Is Available?:
https://blogs.scientificamerican.com/observations/what-if-two-covid-19-victims-need-ventilators-and-just-one-is-available/\
The Globe and Mail – Canadians urged to plan ahead for end-of-life decisions as toll from COVID-19 builds:
https://www.theglobeandmail.com/canada/article-canadians-urged-to-plan-ahead-for-end-of-life-decisions-as-toll-from/
EthicScan Blog – Rationing: Who Gets Care?
http://ethicscan.ca/blog/2020/04/01/rationing-who-gets-care/
National Center for Biotechnology Information – Family Communication at the End of Life:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5618053/
Journal of Medical Ethics – Lack of leadership to limit “futile” end-of-life care leaves Canada hamstrung in COVID-19 pandemic:
https://blogs.bmj.com/medical-ethics/2020/04/29/lack-of-leadership-to-limit-futile-end-of-life-care-leaves-canada-hamstrung-in-covid-19-pandemic/
- Radically Remaking the Future of Transit Industry Post COVID - November 16, 2020
- Radically Remaking the Future of Retailing Industry Post COVID - November 12, 2020
- Radically Remaking the Future of Restaurant Industry Post-COVID - November 12, 2020
